For many women, hot flushes are more than an inconvenience. When they strike at night (as night sweats), they can severely disrupt sleep. During the day, they can cause embarrassment, anxiety, and difficulty concentrating at work. Some women experience several episodes a day; others may have them only occasionally.
Understanding why hot flushes happen is the first step towards finding effective, lasting relief.
Why do hot flushes happen?
Although their exact cause still isn’t fully understood, hot flushes are thought to be the result of changes in the hypothalamus, the part of the brain that regulates the body’s temperature.
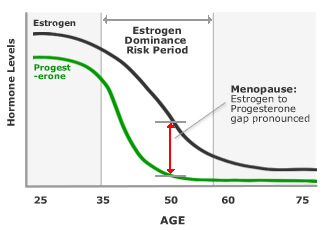
The dramatic drop in hormone levels during menopause — and in particular the imbalance between progesterone and oestrogen known as oestrogen dominance — can cause the hypothalamus to become more sensitive to minor changes in body temperature.
In a woman with balanced hormones, the hypothalamus has a comfortable ‘thermoneutral zone’ — a range of body temperatures it considers normal. During menopause, hormonal changes can narrow this zone dramatically. Even a tiny increase in core temperature can trigger the brain to launch its cooling response as if the body were overheating.
When this happens, blood vessels near the surface of the skin begin to dilate rapidly, increasing blood flow in an attempt to dissipate body heat. This produces the characteristic red, flushed look to the face and neck. The heart may beat faster, and perspiration kicks in to cool the body down. A cold chill often follows a hot flush as the body overshoots in its cooling response, and some women experience only the chill.
How long do hot flushes last?
Individual episodes typically last between 1 and 5 minutes, though they can feel much longer when you are in the middle of one.
As for how long hot flushes continue as a symptom, this varies widely between women. They typically begin during perimenopause — sometimes years before periods stop — and can continue for several years after menopause. For most women, hot flushes last between 2 and 5 years, but some experience them for a decade or more.
The frequency and severity usually decrease over time, particularly when the underlying hormonal imbalance is addressed rather than simply masked.
Night sweats — hot flushes while you sleep
Hot flushes that occur at night are called night sweats. They can be intense enough to soak nightclothes and bedding, disrupting sleep for both the woman and her partner.
The sleep disruption caused by night sweats has a cascading effect on health and wellbeing:
- Fatigue and low energy during the day
- Difficulty concentrating and brain fog
- Irritability and mood swings
- Increased anxiety
- Weakened immune function over time
- Greater susceptibility to weight gain (poor sleep affects hunger hormones)
Addressing night sweats is therefore not just about comfort — it is important for overall health during menopause. See our sleep capsules for additional support alongside hormone balance.
How to get lasting relief from hot flushes
The best treatment for hot flushes is to tackle the source of the problem: hormonal imbalance. Rather than simply managing individual episodes, restoring the balance between progesterone and oestrogen can reduce or eliminate hot flushes at their root.
Supplementation with bioidentical hormones can bring stability back to the hypothalamus, which in turn prevents it from over-reacting to normal temperature fluctuations.
Progesterone supplementation is recommended as a first step. Natural progesterone helps counterbalance oestrogen dominance, which is the underlying driver of most menopausal symptoms including hot flushes.
If hot flushes still persist after progesterone supplementation alone, some bioidentical oestrogen can be added, via a combination cream or a dedicated balancing cream.
Common triggers to avoid
While hormone balance is the long-term solution, there are also practical steps you can take to reduce the frequency and severity of hot flushes by avoiding common triggers.
1. Stress
Stress can be a significant trigger for hot flushes. The stress hormone cortisol can further disrupt hormonal balance and make the hypothalamus more reactive. If certain situations make you anxious, explore relaxation techniques like meditation, deep breathing, and guided imagery. A regular exercise routine can also help keep stress under control.
2. Spicy foods
Diet is generally an important factor in good health, but what you eat can also make a direct difference to your flushes. Spicy food is a common culprit — capsaicin (the compound that gives chillies their heat) can directly trigger the body’s heat-dissipation response. Try to moderate food, sauces, and drinks with a kick, whether that’s Indian or Thai food or just heat from chilli peppers.
3. Caffeine
Your morning cup of coffee may give you a boost of energy, but caffeine and caffeinated drinks — whether hot or cold — may also trigger hot flushes. Caffeine is a stimulant that can increase heart rate and dilate blood vessels.
You can lower your intake by cutting back on coffee, tea, soft, and energy drinks. Although small amounts of dark chocolate have health benefits, don’t forget that caffeine lurks in chocolate too.
4. Alcohol
Drinking alcohol may trigger vasomotor symptoms which lead to hot flushes. When you drink, your blood vessels become dilated and blood flow increases, which can worsen symptoms.
Studies show mixed results, but some experts say it’s best to avoid or reduce alcohol to minimise hot flushes. Take note of whether you’re triggered by all alcohol or just certain types like wine, beer, or spirits.
5. Tobacco
Studies have shown that women smokers had a 1.6-fold increased chance of experiencing hot flushes compared to women who had never smoked. If you smoke cigarettes or vape, your hot flushes may be worse and happen more often. Research suggests that the longer you smoke, and the earlier you start, the more symptoms you may have.
6. Heat and warm environments
Heat is a common and obvious trigger. Normally when your body heats up, brain pathways help to cool you off — but during perimenopause and menopause, the body’s temperature control centre is disrupted, making it over-react.
Reducing the temperature at home, and particularly in the bedroom, can make a real difference. Many women find that keeping a window open, using a fan, or reducing central heating helps significantly.
7. Clothing choices
Tight clothing can be an issue, as even small increases in your core body temperature may set off symptoms. Try to keep your body cool by choosing clothing made of natural fibres, which are more breathable than synthetic fabrics.
Dressing in loose layers helps too — when your body temperature starts to rise, you can easily peel them off to cool down. This is especially useful at work or in social situations where you may want to manage symptoms discreetly.
Hot flushes and hot flashes — the same thing
If you have been searching for information, you may have encountered both ‘hot flushes’ and ‘hot flashes’. These are the same symptom — ‘hot flushes’ is the standard British English term, while ‘hot flashes’ is the American English equivalent.
When to seek further help
While hot flushes are a normal part of the menopausal transition, they should not be dismissed as something you simply have to endure. If your hot flushes are severely affecting your quality of life, your sleep, your work, or your relationships, it is worth speaking to your healthcare professional.
Wellsprings Serenity is a premium natural progesterone cream that has been helping women find relief from hot flushes and other menopause symptoms since 1997. Read the stories of women who have found relief, and learn more about natural progesterone in our Hormone Learning section.
References
- Rushton, A. & Bond, Dr S. Natural Progesterone. Wellsprings Health.
- Lee, J.R. (1993). Natural Progesterone: The Multiple Roles of a Remarkable Hormone. BLL Publishing.
Medical Disclaimer
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
This article is for general informational purposes only and is not intended as medical advice. It should not be used to diagnose or treat any health condition. Always consult your doctor or qualified healthcare professional before starting any new treatment or making changes to your existing care. Every woman is unique and individual results may vary.
Menopause and Weight Gain
Menopause, Progesterone and Gut Health
Find out what causes this common symptom, and how to get relief
Progesterone supplementation can naturally boost gut health
Hear what doctors have to say about natural progesterone and its benefits
Natural progesterone can be an effective treatment for this serious condition
What happens to hormones at menopause and how can symptoms be treated?
Understand what's behind the increased incidence of oestrogen dominance in the western world
How can a cream deliver progesterone into the body?
What are bioidentical hormones and why are they relevant to your health
Learn how to get the most from your Wellsprings bioidentical hormone creams with proper application techniques, timing, and usage guidelines
Wellsprings offers two varieties of natural progesterone cream. Read on to find out which is best for you
Oestrogen dominance can interfere with thyroid hormone activity
Despite claims to the contrary, Yam Extract does NOT contain progesterone or raise progesterone levels in the body
All information given on this site is for general interest only. Every woman is unique. Your results may vary.